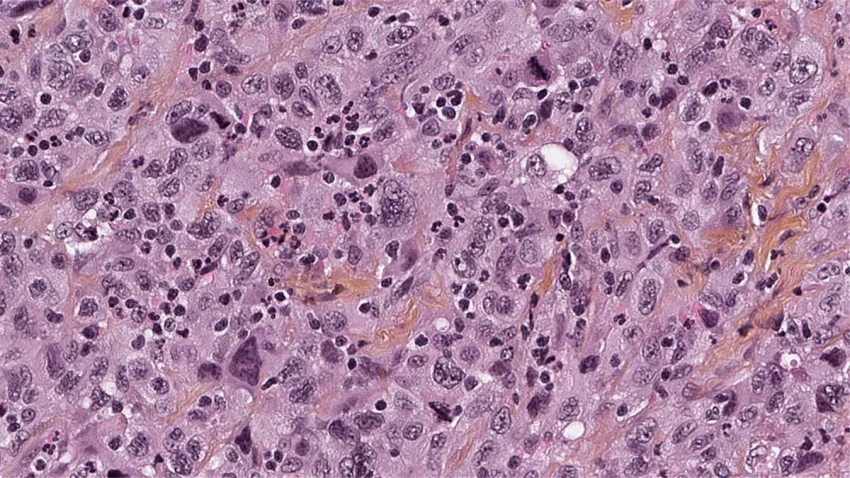
Peritoneal mesothelioma pathology outlines are crucial for understanding this rare and aggressive cancer. As a challenging disease to diagnose and treat, it’s essential for healthcare professionals and patients alike to grasp its complexities. This guide dives deep into the pathological features, diagnostic approaches, and treatment strategies for peritoneal mesothelioma. We’ll explore everything from its cellular origins to cutting-edge therapies, shedding light on this often-overlooked form of cancer.
Key Takeaways:
- Peritoneal mesothelioma primarily affects the lining of the abdominal cavity
- Asbestos exposure is a major risk factor, but not the only cause
- Histological subtypes include epithelioid, sarcomatoid, and biphasic
- Diagnosis often involves imaging, biopsy, and pathological evaluation
- Treatment may include cytoreductive surgery, HIPEC, and systemic chemotherapy
Let’s embark on this journey to unravel the intricacies of peritoneal mesothelioma, arming ourselves with knowledge to better understand and combat this formidable disease.
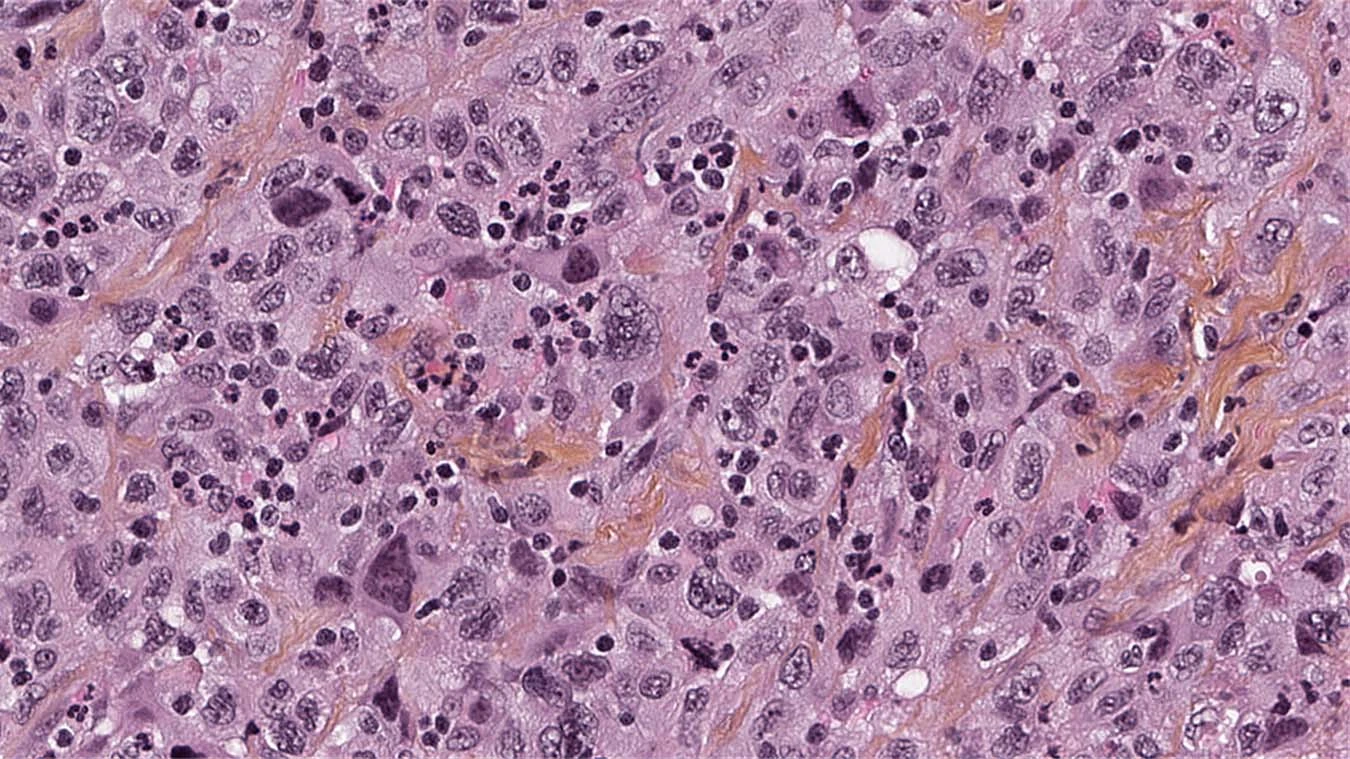
Understanding Peritoneal Mesothelioma
Peritoneal mesothelioma is a rare cancer affecting the peritoneum, the lining of the abdominal cavity. It accounts for 7-30% of all mesothelioma cases, with an average incidence of 1.94 cases per 100,000 men and 0.41 cases per 100,000 women in the United States. While asbestos exposure is a known risk factor, the correlation is weaker compared to pleural mesothelioma.
Histological Subtypes
Three main histological subtypes characterize peritoneal mesothelioma:
- Epithelioid: Most common, accounting for about 75% of cases
- Sarcomatoid: Least common, making up roughly 10% of cases
- Biphasic: A combination of epithelioid and sarcomatoid, representing about 15% of cases
Understanding these subtypes is crucial for prognosis and treatment planning, as epithelioid mesothelioma generally has a better outlook than sarcomatoid or biphasic types.
Diagnostic Approaches in Peritoneal Mesothelioma
Diagnosis of peritoneal mesothelioma is often challenging due to its nonspecific symptoms. Patients typically present with abdominal distension and pain, which can be mistaken for other conditions.
Imaging Techniques
CT scans are the primary imaging tool, but no single imaging method is definitive for peritoneal mesothelioma. Other techniques include:
- MRI: Provides detailed soft tissue images
- PET scans: Useful for detecting metabolic activity in tumors
Biopsy and Pathological Evaluation
Confirmation of diagnosis requires pathological evaluation, often through:
- Fine-needle aspiration
- Laparoscopic biopsy
These procedures allow for histological examination and immunohistochemical staining, essential for accurate diagnosis and subtype determination.
Treatment Strategies Based on Pathology
Treatment approaches vary based on the pathological findings and disease stage.
Cytoreductive Surgery and HIPEC
This combination is the first-line treatment for selected patients. Studies report median survival rates ranging from 30 to 92 months, depending on the completeness of cytoreduction. The procedure involves:
- Surgical removal of visible tumors
- Application of heated chemotherapy directly to the abdominal cavity
Systemic Chemotherapy
For patients who are not surgical candidates, systemic chemotherapy is the primary treatment option. The standard regimen includes:
- Pemetrexed combined with cisplatin or carboplatin
Clinical trials have shown varying efficacy, with response rates ranging from 20% to 40%.
Challenges in Peritoneal Mesothelioma Management
Several challenges complicate the management of peritoneal mesothelioma:
- Late-stage diagnosis: Due to vague initial symptoms, diagnosis often occurs at advanced stages
- Treatment resistance: Some tumors develop resistance to standard chemotherapy regimens
- High recurrence rates: Even after successful initial treatment, recurrence is common
Overcoming Challenges
To address these issues, researchers are exploring:
- Targeted therapies based on molecular profiling
- Immunotherapy approaches
- Improved early detection methods
Case Study: Benign Multicystic Peritoneal Mesothelioma
A 62-year-old woman presented with diffuse abdominal pain, initially diagnosed with an incarcerated incisional hernia. During surgery, several cystic masses were discovered in the abdomen:
- A 6 cm x 5 cm x 4 cm cystic mass in the right ovary
- Four small cysts in the small bowel
- An 11 cm x 10 cm x 3 cm retroperitoneal cyst
Complete resection of these lesions confirmed the diagnosis of benign multicystic peritoneal mesothelioma (BMPM). The patient recovered well and remained symptom-free for two years post-surgery.
This case highlights the importance of thorough surgical exploration and pathological examination in diagnosing and treating peritoneal mesotheliomas, even in their benign forms.
Best Practices for Pathologists and Clinicians
To improve outcomes for patients with peritoneal mesothelioma, healthcare professionals should:
- Follow standardized reporting guidelines for pathology
- Adopt a multidisciplinary approach to patient care
- Stay updated on advancements in diagnosis and treatment through continuing education
By adhering to these best practices, clinicians can ensure more accurate diagnoses, tailored treatment plans, and potentially improved patient outcomes in the challenging landscape of peritoneal mesothelioma management.

Conclusion
Peritoneal mesothelioma pathology outlines serve as a crucial roadmap in navigating this complex disease. As we’ve explored, from its cellular intricacies to cutting-edge treatments, understanding the pathological nuances is key to improving patient outcomes. While challenges persist, the future holds promise. Emerging therapies, coupled with refined diagnostic techniques, offer hope for earlier detection and more effective management. As research progresses, we may see a shift towards personalized treatment plans based on individual tumor profiles. For healthcare professionals, staying informed and embracing multidisciplinary approaches will be paramount. For patients and their families, this knowledge empowers informed decision-making. Together, we’re paving the way for a future where peritoneal mesothelioma, though formidable, becomes increasingly manageable.