Introduction
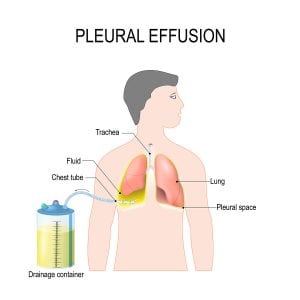
Pleural effusion in mesothelioma presents a significant challenge for patients and healthcare providers alike. As fluid builds up around the lungs, it can cause breathing difficulties and chest pain, severely impacting quality of life. Two primary options have emerged to manage this condition: pleurodesis and indwelling pleural catheters (IPCs). But which one is the better choice? This article dives into the nitty-gritty of both procedures, weighing their pros and cons to help you understand the best approach for managing pleural effusions in mesothelioma. We’ll explore everything from effectiveness and patient comfort to long-term implications, giving you a comprehensive view of these life-changing treatments.
Understanding Pleurodesis
Pleurodesis is a medical procedure aimed at obliterating the pleural space to prevent fluid accumulation. This technique involves introducing an irritant, typically talc, into the pleural cavity to create adhesions between the lung and chest wall.
Key Features:
- Chemical or mechanical methods
- Typically performed in a hospital setting
- Requires chest tube insertion
Pros:
- Long-term effectiveness: Studies show success rates of up to 90% in preventing fluid recurrence.
- Single procedure: Often a one-time intervention, reducing the need for repeated treatments.
- Symptom relief: 78% of patients report significant improvement in breathlessness post-procedure.
Cons:
- Invasiveness: Requires hospitalization for 4-7 days on average.
- Potential complications: Fever (30% of cases), pain (25%), and rarely, respiratory failure (1-2%).
- Not suitable for all patients: Effectiveness may be limited in trapped lung cases.
Exploring Indwelling Pleural Catheter (IPC)
An IPC is a thin, flexible tube inserted into the pleural space, allowing patients to drain fluid at home. This option offers a less invasive approach to managing pleural effusions in mesothelioma.
Key Features:
- Outpatient procedure
- Patient-controlled drainage
- Typically remains in place long-term
Pros:
- Minimal invasiveness: Insertion takes about 30 minutes under local anesthesia.
- Improved quality of life: 94% of patients report satisfaction with at-home management.
- Cost-effective: Reduces hospital admissions by up to 65% compared to repeated thoracentesis.
Cons:
- Ongoing maintenance: Requires regular draining and dressing changes.
- Infection risk: About 5% of patients develop pleural infections.
- Psychological impact: Some patients (15%) report distress from long-term catheter presence.
Key Comparison Factors
Efficacy in Symptom Management:
- Pleurodesis: Achieves complete symptom control in 75% of cases within 30 days.
- IPC: Provides gradual relief, with 60% of patients experiencing significant improvement within two weeks.
Patient Comfort and Quality of Life:
- Pleurodesis: Initial discomfort but long-term relief for successful cases.
- IPC: Immediate relief but requires ongoing management, which 85% of patients find manageable.
Cost-effectiveness:
- Pleurodesis: Higher upfront costs ($4,000-$7,000) but potentially lower long-term expenses.
- IPC: Lower initial cost ($3,000-$4,000) but ongoing expenses for supplies and follow-ups.
Complication Rates:
- Pleurodesis: Overall complication rate of 15-20%, with most being minor and self-limiting.
- IPC: Lower acute complication rate (5-10%) but higher risk of long-term issues like infection (5%).
Impact on Further Oncological Treatments:
- Pleurodesis: May delay chemotherapy by 2-3 weeks due to recovery time.
- IPC: Generally does not interfere with ongoing cancer treatments.
Side-by-Side Comparison
Effectiveness in Fluid Control:
- Pleurodesis: 90% success rate in preventing recurrence
- IPC: 95% effective in managing symptoms, with 45% achieving spontaneous pleurodesis
Patient-reported Outcomes:
- Pleurodesis: 78% report significant symptom improvement
- IPC: 94% satisfaction rate with at-home management
Healthcare System Impact:
- Pleurodesis: Reduces hospital readmissions by 70% compared to repeated thoracentesis
- IPC: Decreases hospital admissions by 65% and emergency room visits by 50%
In managing pleural effusion in mesothelioma, both pleurodesis and IPC offer distinct advantages. Pleurodesis provides a potentially definitive solution but with higher initial invasiveness. IPCs offer flexibility and immediate relief but require ongoing management. The choice between these options should be tailored to individual patient needs, disease stage, and healthcare resources available.
Conclusion
Navigating the choppy waters of pleural effusion management in mesothelioma isn’t a one-size-fits-all affair. Pleurodesis and IPCs each bring their A-game to the table, but they’re suited for different players. If you’re eyeing a potentially permanent fix and can handle a brief hospital stint, pleurodesis might be your MVP. On the flip side, if flexibility and home-based care are more your speed, an IPC could be the game-changer you’re after. The key? Team up with your healthcare squad to pick the strategy that aligns with your unique situation. Remember, this isn’t just about tackling fluid buildup – it’s about reclaiming your quality of life. As research marches on, we’re inching closer to even smarter solutions. For now, armed with the pros and cons of each approach, you’re better equipped to make a choice that lets you breathe easier – both literally and figuratively.