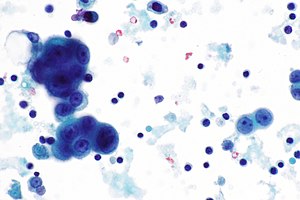
Peritoneal mesothelioma, a rare and aggressive cancer affecting the abdominal lining, presents significant challenges in diagnosis and treatment. This comprehensive outline of peritoneal mesothelioma pathology explores the disease’s epidemiology, diagnostic methods, and treatment modalities. With an incidence of 0.5-3 cases per million population annually, peritoneal mesothelioma accounts for 10-30% of all mesothelioma cases. The disease’s rarity and non-specific symptoms often result in delayed diagnosis, averaging 4-6 months from symptom onset to confirmation. This delay significantly impacts patient outcomes, with a 5-year survival rate of only 20-30%.
Recent advancements in imaging techniques and immunohistochemistry have improved diagnostic accuracy. CT scans, the primary imaging modality, typically reveal heterogeneous soft tissue masses with ascites in 30-80% of cases. Histopathological evaluation remains the gold standard, classifying peritoneal mesothelioma into three subtypes: epithelioid (75% of cases), sarcomatoid, and biphasic. Immunohistochemical markers like calretinin and WT1 enhance diagnostic precision, with up to 95% sensitivity in distinguishing mesothelioma from other malignancies.
The economic burden of peritoneal mesothelioma is substantial, with treatment costs exceeding $500,000 per patient. Emerging treatments, such as cytoreductive surgery (CRS) combined with heated intraperitoneal chemotherapy (HIPEC), show promise, with median survival rates ranging from 30 to 92 months. Ongoing research focuses on molecular targets for personalized therapy and early detection methods, offering hope for improved outcomes in this challenging malignancy.
Current State of Peritoneal Mesothelioma Pathology
Recent advancements in imaging techniques and immunohistochemistry have significantly improved the accuracy of peritoneal mesothelioma diagnosis. CT scans, serving as the first-line imaging modality, typically reveal heterogeneous soft tissue masses with associated ascites in 30-80% of cases. Histopathological evaluation remains the gold standard for diagnosis, with the World Health Organization classifying peritoneal mesothelioma into three main subtypes:
- Epithelioid (75% of cases)
- Sarcomatoid
- Biphasic/mixed
The use of immunohistochemical markers, such as calretinin and WT1, has enhanced diagnostic accuracy, with a sensitivity of up to 95% in distinguishing mesothelioma from other malignancies.
Impact Analysis of Peritoneal Mesothelioma
The impact of peritoneal mesothelioma extends beyond individual patients to healthcare systems and society at large. The disease predominantly affects individuals with a history of asbestos exposure, with a latency period of 20-50 years. This long latency period complicates epidemiological studies and prevention efforts.
The economic burden of peritoneal mesothelioma is substantial, with treatment costs estimated to exceed $500,000 per patient. Additionally, the psychological impact on patients and their families is profound, given the poor prognosis and limited treatment options.
Challenges in Peritoneal Mesothelioma Pathology
Diagnosing peritoneal mesothelioma presents several challenges:
- Non-specific symptoms, including abdominal pain (27-58% of cases) and distension (30-80% of cases), often lead to misdiagnosis or delayed diagnosis
- The rarity of the disease means many clinicians lack experience in recognizing and managing it effectively
- Development of effective treatment strategies is hindered by the heterogeneity of the disease and its resistance to conventional chemotherapy regimens
Future Directions in Peritoneal Mesothelioma Treatment
Emerging treatment modalities offer hope for improved outcomes in peritoneal mesothelioma:
- Cytoreductive surgery (CRS) combined with heated intraperitoneal chemotherapy (HIPEC) has shown promise, with median survival rates ranging from 30 to 92 months in various institutional studies
- Ongoing research focuses on identifying molecular targets for personalized therapy, with drugs targeting pathways such as VEGF and PD-1/PD-L1 showing potential
- Efforts to develop early detection methods, including the use of biomarkers like mesothelin and osteopontin, may lead to earlier diagnosis and improved survival rates
As research progresses, improvements in early detection, accurate diagnosis, and targeted therapies offer hope for better outcomes in peritoneal mesothelioma pathology.
Conclusion
Peritoneal mesothelioma pathology outlines reveal a complex and challenging malignancy that demands continued research and clinical attention. The rarity of the disease, coupled with its non-specific symptoms, underscores the importance of accurate diagnostic methods and comprehensive pathological understanding. Advancements in imaging techniques, immunohistochemistry, and treatment modalities, particularly CRS-HIPEC, have improved patient outcomes, with median survival rates now reaching up to 92 months in some cases. However, the economic burden and psychological impact on patients remain significant challenges. As we look to the future, the focus on molecular targets and early detection methods offers hope for more personalized and effective treatments. By continuing to refine our understanding of peritoneal mesothelioma pathology, we can work towards improving diagnosis, treatment, and ultimately, patient survival rates in this rare but devastating disease.
References
- Bridda A, et al. Peritoneal mesothelioma: a review. MedGenMed. 2007;9(2):32.
- Husain AN, et al. Guidelines for pathologic diagnosis of malignant mesothelioma: 2017 update of the consensus statement from the International Mesothelioma Interest Group. Arch Pathol Lab Med. 2018;142(1):89-108.
- Deraco M, et al. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy for malignant peritoneal mesothelioma: multi-institutional experience. J Clin Oncol. 2012;30(36):4512-4518.
- Cao S, et al. Advances in malignant peritoneal mesothelioma. Int J Colorectal Dis. 2015;30(1):1-10.
- Boffetta P. Epidemiology of peritoneal mesothelioma: a review. Ann Oncol. 2007;18(6):985-990.