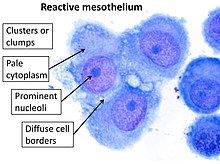
Mesothelial cells in pleural fluid play a crucial role in maintaining lung health and can serve as vital indicators of various respiratory conditions. These microscopic sentinels line the pleural cavity, forming a protective barrier and contributing to the delicate balance of fluids surrounding our lungs. As we delve into the world of these cellular guardians, we’ll uncover their significance in both normal lung function and disease states. From their role in immune responses to their potential as diagnostic tools, mesothelial cells offer a fascinating glimpse into the complex workings of our respiratory system.Key Takeaways:
- Mesothelial cells maintain pleural homeostasis and regulate fluid balance
- They act as a first line of defense against pathogens and inflammation
- Changes in mesothelial cells can indicate various pleural diseases
- Cytological examination of these cells aids in diagnosing respiratory conditions
- Mesothelial cells show promise as biomarkers and therapeutic targets
Understanding Mesothelial Cells and Pleural Fluid
Mesothelial cells are specialized epithelial-like cells that originate from the embryonic mesoderm. These cells, typically 10-50 μm in diameter, form a monolayer called the mesothelium, which lines the pleural, peritoneal, and pericardial cavities. In the context of pleural health, mesothelial cells play a pivotal role in maintaining the delicate balance of the pleural environment.
Pleural fluid, a thin layer of liquid between the visceral and parietal pleura, is primarily composed of water, electrolytes, and proteins. This fluid facilitates smooth movement of the lungs during respiration and helps maintain negative pressure in the pleural space. Normal pleural fluid volume ranges from 0.1 to 0.2 mL/kg body weight, with a protein content of less than 1.5 g/dL.
Functions of Mesothelial Cells in the Pleural Cavity
Mesothelial cells serve multiple critical functions:
- Barrier function: They form a nonadhesive, protective surface that prevents organ adhesion.
- Fluid regulation: These cells actively participate in the transport of fluid and solutes across the pleural membrane.
- Immune response: Mesothelial cells contribute to both innate and adaptive immunity.
- Tissue repair: They play a role in wound healing and tissue regeneration.
The Importance of Mesothelial Cells in Pleural Health
Mesothelial cells are crucial for maintaining pleural homeostasis and defending against various pathological conditions. Their importance is underscored by their multifaceted roles in pleural health.
Barrier Function and Protection
The mesothelial layer acts as a physical barrier, preventing adhesions between organs and protecting against invading pathogens. Studies have shown that mesothelial cells express various adhesion molecules and junctional proteins, such as E-cadherin and β-catenin, which are essential for maintaining this protective barrier.
Immune Response Regulation
Mesothelial cells exhibit both innate and adaptive immunity mechanisms. They express Toll-like receptors (TLRs) that recognize pathogen-associated molecular patterns, triggering the release of pro-inflammatory cytokines and chemokines. Research has demonstrated that mesothelial cells can produce up to 40 different cytokines and growth factors in response to various stimuli.
Tissue Repair and Regeneration
In response to injury, mesothelial cells can undergo epithelial-to-mesenchymal transition (EMT), a process that allows them to adopt a more fibroblast-like phenotype. This transition is crucial for wound healing and tissue remodeling. Studies have shown that up to 80% of new mesothelial cells during peritoneal repair may originate from this EMT process.
Mesothelial Cells as Indicators of Pleural Diseases
Changes in mesothelial cell morphology and behavior can serve as important indicators of various pleural diseases.
Pleural Effusions
Pleural effusions, characterized by excess fluid accumulation in the pleural space, can be classified as transudates or exudates. In exudative effusions, mesothelial cells often appear reactive, with increased size and nuclear-to-cytoplasmic ratio. Approximately 15-20% of all pleural effusions are malignant, highlighting the importance of mesothelial cell analysis in diagnosis.
Malignant Pleural Diseases
In malignant pleural mesothelioma, a rare but aggressive cancer, mesothelial cells undergo malignant transformation. Diagnosis often relies on cytological examination of pleural fluid, where atypical mesothelial cells may be observed. Mesothelioma has a poor prognosis, with a median survival of only 9-17 months after diagnosis.
Inflammatory Conditions
In inflammatory conditions like pleuritis or tuberculosis pleurisy, mesothelial cells exhibit characteristic changes. These may include increased cell size, prominent nucleoli, and cytoplasmic vacuolation. In tuberculosis pleurisy, for instance, the pleural fluid typically contains a high proportion of lymphocytes (>50%) alongside reactive mesothelial cells.
Challenges in Mesothelial Cell Analysis
While mesothelial cells provide valuable diagnostic information, their analysis comes with certain challenges.
Differentiation from Other Cell Types
One of the primary challenges is distinguishing mesothelial cells from other cell types, particularly adenocarcinoma cells. Both can appear similar under light microscopy, with a misdiagnosis rate of up to 15% reported in some studies. Immunohistochemistry techniques using markers such as calretinin and WT1 have improved accuracy, reducing misdiagnosis rates to below 5% in experienced laboratories.
Sampling and Processing Issues
Adequate specimen collection and preservation are crucial for accurate analysis. Studies have shown that delays in processing of more than 1 hour can lead to significant cellular degeneration, potentially affecting diagnostic accuracy by up to 20%.
Future Perspectives and Research Directions
Ongoing research is exploring the potential of mesothelial cells as biomarkers for disease activity and as therapeutic targets. Recent studies have suggested that certain mesothelial cell markers, such as mesothelin, may have up to 95% specificity in diagnosing malignant pleural mesothelioma.
Advancements in mesothelial cell analysis techniques, including the use of artificial intelligence in cytological examination, show promise in improving diagnostic accuracy. Early studies indicate that AI-assisted analysis could potentially increase diagnostic sensitivity by up to 15-20% compared to traditional methods.
Conclusion: Mesothelial Cells – Tiny Guardians with Big Potential
Mesothelial cells in pleural fluid are far more than just passive lining cells. They’re dynamic, multifaceted guardians of our respiratory health, playing crucial roles in maintaining pleural balance, fighting off infections, and even serving as early warning systems for various lung diseases. As our understanding of these microscopic sentinels grows, so does their potential in medical diagnostics and treatments. From improving early detection of pleural diseases to potentially developing targeted therapies, mesothelial cells are opening up exciting new avenues in pulmonary medicine. While challenges in their analysis persist, ongoing advancements in technology and research methods are steadily overcoming these hurdles. As we continue to unlock the secrets of mesothelial cells, we’re not just gaining insights into lung health – we’re paving the way for more effective, personalized approaches to respiratory care. The future of pulmonary medicine looks brighter, thanks to these tiny yet mighty cellular guardians.