Malignant mesothelioma pleural effusion is a challenging complication that affects many patients with this aggressive cancer. As the disease progresses, fluid accumulates in the space between the lungs and chest wall, leading to discomfort and breathing difficulties. This article delves into the intricate relationship between mesothelioma and pleural effusion, exploring its causes, diagnosis, and management options. We’ll unpack the complexities of this condition, shedding light on the latest treatments and offering insights for patients and caregivers navigating this difficult journey.
Key Takeaways:
- Pleural effusion is a common symptom in mesothelioma patients
- Diagnosis involves imaging techniques and fluid analysis
- Treatment options range from palliative care to long-term management strategies
- Recurrence and quality of life impact are significant challenges
- Multidisciplinary care is crucial for comprehensive patient support
Understanding Malignant Mesothelioma
Malignant mesothelioma is a rare and aggressive cancer primarily affecting the pleura, the thin membrane lining the lungs and chest cavity. Approximately 3,300 new cases are diagnosed annually in the U.S., with pleural mesothelioma accounting for about 80% of all mesothelioma diagnoses.
Types and Causes
There are three main types of mesothelioma:
- Epithelioid (60-80% of cases)
- Sarcomatoid (10%)
- Biphasic (10-15%)
Asbestos exposure is responsible for about 70% of mesothelioma cases. The risk increases significantly in occupations involving asbestos, such as construction, shipbuilding, and firefighting. Other potential causes include radiation exposure and genetic mutations.
Pleural Effusion in Mesothelioma
Pleural effusion, the abnormal buildup of fluid in the pleural space, affects over 95% of mesothelioma patients at some point during their illness. This complication occurs due to increased vascular permeability and impaired lymphatic drainage caused by the tumor.
Types of Pleural Effusion
In mesothelioma, pleural effusions are typically exudative, meaning they result from direct pleural involvement. These effusions are often cloudy and contain cells and proteins. Malignant pleural effusions account for 54-90% of cases in mesothelioma patients.
Diagnosis of Malignant Mesothelioma Pleural Effusion
Accurate diagnosis is crucial for effective management. The diagnostic process typically involves:
Imaging Techniques
- Chest X-rays
- CT scans
- MRI
These imaging methods can detect effusions and associated malignancies with high accuracy.
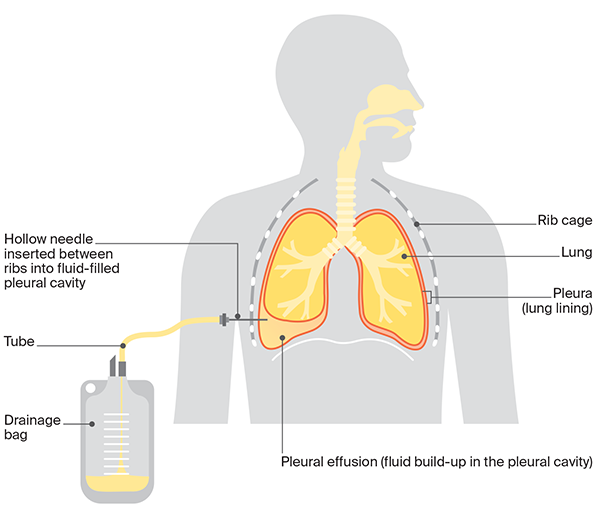
Thoracentesis and Fluid Analysis
Thoracentesis, a procedure to extract pleural fluid, serves both diagnostic and therapeutic purposes. However, cytology has low sensitivity for confirming mesothelioma, with accuracy rates varying between studies.
Biopsy Procedures
Histological analysis through biopsies, particularly those guided by imaging, significantly enhances diagnostic accuracy. Video-Assisted Thoracoscopic Surgery (VATS) offers the ability to perform biopsies with reduced complication rates.
Treatment Options
Management of malignant mesothelioma pleural effusion focuses on symptom relief and preventing fluid recurrence.
Palliative Treatments
- Thoracentesis: Provides immediate relief but often requires repeated procedures.
- Indwelling Pleural Catheters (IPC): Recommended for recurrent effusions, allowing patients to manage drainage at home.
Long-term Management Strategies
- Pleurodesis: Uses sclerosing agents, typically talc, to obliterate the pleural space. Success rates in mesothelioma are lower than in other malignancies, at approximately 30%.
- Pleurectomy/Decortication: Surgical removal of affected pleura, which can be effective but carries higher risks.
Systemic Treatments
Chemotherapy, particularly the combination of pemetrexed and cisplatin, is the standard first-line treatment, improving survival rates. Immunotherapy and targeted therapies like bevacizumab show promise in conjunction with chemotherapy.
Challenges and Complications
Managing malignant mesothelioma pleural effusion presents several challenges:
- Recurrence: Pleural effusions often recur, necessitating repeated interventions.
- Quality of Life Impact: Symptoms like dyspnea and chest pain significantly affect patient wellbeing.
- Treatment-related Side Effects: Procedures and medications can cause complications and discomfort.
- Psychological Burden: Living with a terminal illness and its symptoms takes a toll on mental health.
Patient Care and Support
Comprehensive care is essential for mesothelioma patients with pleural effusion. This includes:
- Multidisciplinary Team Approach: Involving oncologists, pulmonologists, and palliative care specialists.
- Pain Management: Tailored strategies to alleviate discomfort.
- Nutritional Support: Maintaining proper nutrition to support treatment and quality of life.
- Emotional and Psychological Support: Counseling and support groups to address the mental health aspects of the disease.
Case Study: Managing Malignant Mesothelioma Pleural Effusion
A 57-year-old male presented with dyspnea and left-sided chest pain for 15 days. Despite no history of asbestos exposure, imaging revealed left-sided pleural effusion. Initial treatment for suspected infection was ineffective. Further examination, including thoracotomy and lung biopsy, confirmed mesothelioma diagnosis. This case highlights the importance of thorough investigation even in the absence of typical risk factors.
Conclusion: Navigating the Complexities of Malignant Mesothelioma Pleural Effusion
Malignant mesothelioma pleural effusion presents a formidable challenge in cancer care, demanding a nuanced approach to diagnosis and treatment. As we’ve explored, this condition significantly impacts patient quality of life, necessitating a delicate balance between symptom management and long-term strategies. The landscape of mesothelioma treatment is evolving, with promising advancements in immunotherapy and targeted therapies offering new hope. Yet, the importance of personalized care cannot be overstated. Each patient’s journey is unique, and tailoring interventions to individual needs is crucial. Looking ahead, the integration of cutting-edge research with compassionate, patient-centered care holds the key to improving outcomes. As we continue to unravel the complexities of this condition, the focus remains on enhancing quality of life and extending survival for those affected by this challenging disease.