Surgery for pleural mesothelioma plays a crucial role in managing this rare and aggressive cancer. As patients and their loved ones grapple with treatment decisions, understanding the surgical landscape becomes paramount. From curative procedures aimed at tumor removal to palliative interventions for symptom relief, each option carries its own set of benefits and challenges. This comprehensive guide delves into the world of mesothelioma surgery, exploring everything from patient eligibility to emerging techniques. Whether you’re newly diagnosed or seeking alternative treatments, this article aims to equip you with the knowledge to make informed decisions about your care.
Key Takeaways:
- Surgical options range from aggressive tumor removal to symptom management
- Patient eligibility depends on cancer stage, overall health, and tumor characteristics
- Surgery can improve survival rates and quality of life for suitable candidates
- Multimodal therapy often combines surgery with chemotherapy or radiation for optimal outcomes
- Ongoing research is paving the way for less invasive and more effective surgical techniques
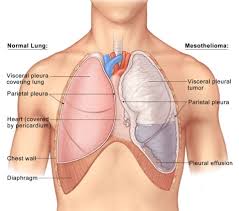
Understanding Pleural Mesothelioma
Pleural mesothelioma is a rare and aggressive cancer affecting the lining of the lungs. It’s primarily caused by asbestos exposure, with a latency period of 20-50 years. According to the American Cancer Society, approximately 3,000 new cases are diagnosed annually in the United States, accounting for 75% of all mesothelioma cases.
Diagnosis and Staging Challenges
Early diagnosis is crucial but challenging due to non-specific symptoms. Staging is typically done using the TNM system, with stage I-IV classifications determining treatment options and prognosis. Only about 20% of patients are diagnosed at stages I or II, when surgery is most effective.
Surgical Options for Pleural Mesothelioma
Curative Surgical Procedures
Extrapleural Pneumonectomy (EPP): This aggressive surgery removes the affected lung, pleura, diaphragm, and pericardium. While potentially curative, it carries significant risks. Studies show a median survival rate of 15 months post-EPP.
Pleurectomy/Decortication (P/D): A less radical option, P/D removes the pleural lining and visible tumors while preserving the lung. It offers a median survival of 22 months and is associated with fewer complications than EPP.
Palliative Surgical Interventions
Pleurodesis: This procedure aims to prevent fluid buildup in the pleural space, improving breathing and quality of life. Success rates for pleurodesis range from 80-90%.
Thoracentesis: A minimally invasive procedure to drain excess fluid, offering immediate symptom relief. However, fluid often recurs, necessitating repeated procedures in 90% of cases.
Eligibility and Patient Selection
Surgical candidacy depends on various factors:
- Cancer stage (typically stages I-III)
- Overall health and lung function
- Tumor cell type (epithelioid has better surgical outcomes)
- Age (patients under 70 generally tolerate surgery better)
A multidisciplinary team assessment is crucial, involving oncologists, surgeons, and pulmonologists. Only 15-20% of patients typically qualify for major surgery.
Benefits and Risks of Mesothelioma Surgery
Potential Advantages
- Improved survival rates: Up to 24% of early-stage patients achieve 5-year survival post-surgery
- Enhanced quality of life through symptom management
- Opportunity for multimodal therapy, improving overall outcomes
Associated Risks and Complications
- 30-day mortality rates: 3-4% for P/D, 7% for EPP
- Major complications in up to 30% of cases, including pneumonia and cardiac issues
- Long-term effects on lung function, particularly with EPP
Recovery and Post-Operative Care
Recovery timelines vary:
- Hospital stays: 7-15 days on average
- Full recovery: 4-8 weeks for P/D, 3-6 months for EPP
Comprehensive rehabilitation, including respiratory therapy and pain management, is crucial for optimal recovery. Follow-up treatments often include chemotherapy or radiation to address residual cancer cells.
Multimodal Therapy Approach
Combining surgery with other treatments significantly improves outcomes:
- Neoadjuvant therapy (pre-surgery): Can shrink tumors, making surgery more effective
- Adjuvant therapy (post-surgery): Targets residual cancer cells, reducing recurrence risk
- Studies show multimodal approaches can extend median survival to 29 months or more
Emerging Surgical Techniques and Research
Ongoing advancements are shaping the future of mesothelioma surgery:
- Minimally invasive techniques reducing recovery times and complications
- Intraoperative therapies like heated chemotherapy showing promise in clinical trials
- Immunotherapy combinations being explored to enhance surgical outcomes
The MARS-2 trial, set to conclude in 2023, aims to definitively compare surgery plus chemotherapy against chemotherapy alone, potentially reshaping treatment paradigms.
Conclusion: Navigating the Future of Mesothelioma Treatment
As we’ve explored the landscape of surgery for pleural mesothelioma, it’s clear that this field is rapidly evolving. While surgical interventions offer hope for many patients, they’re just one piece of a complex treatment puzzle. The future of mesothelioma care lies in personalized approaches that consider each patient’s unique circumstances. Emerging technologies, like AI-assisted surgical planning and targeted therapies, promise to refine our strategies further. But beyond the operating room, we must also focus on prevention and early detection. By raising awareness about asbestos risks and improving screening methods, we can catch this insidious disease earlier, when treatment is most effective. As research progresses, the outlook for mesothelioma patients continues to improve, offering a glimpse of a future where this once-devastating diagnosis becomes increasingly manageable.