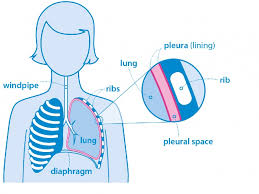
Malignant pleural mesothelioma prognosis remains a challenging aspect of this rare and aggressive cancer. As patients and their loved ones grapple with treatment decisions, understanding the pros and cons of various approaches becomes crucial. This article dives into the heart of the matter, comparing surgical interventions like pleurectomy/decortication and extrapleural pneumonectomy with non-surgical options such as chemotherapy and radiation therapy. We’ll explore how these choices impact survival rates, quality of life, and overall patient outcomes. By examining key prognostic factors and emerging therapies, we aim to provide a comprehensive view of the current landscape in mesothelioma management. Whether you’re facing this diagnosis or simply seeking to understand more, this comparison will shed light on the complex world of mesothelioma prognosis and treatment.
Surgical Interventions for Malignant Pleural Mesothelioma
Pleurectomy/Decortication (P/D)
P/D is a lung-sparing surgery that removes the pleural lining and visible tumors. It’s typically recommended for early-stage patients with good overall health.
Advantages of P/D
- Preserves lung function, with up to 90% of patients experiencing improved breathing post-surgery
- Lower mortality rate (2-3%) compared to more aggressive surgeries
- Potential for improved quality of life, with 60-70% of patients reporting reduced symptoms
Potential Drawbacks and Risks
- May not remove all microscopic cancer cells, leading to a 50-60% recurrence rate within 2 years
- Limited to earlier stage patients, excluding approximately 70% of diagnosed cases
- Requires extensive recovery period, typically 4-6 weeks
Extrapleural Pneumonectomy (EPP)
EPP is a more aggressive surgery that removes the affected lung, pleura, diaphragm, and pericardium. It’s considered for patients with more advanced disease but good overall health.
Benefits of EPP
- More complete tumor removal, potentially improving survival rates by 20-30%
- Can be combined with radiation therapy for enhanced local control
- May offer longer disease-free intervals for select patients
Limitations and Complications
- Higher mortality rate (4-7%) compared to P/D
- Significant decrease in lung function, impacting quality of life
- Extended recovery period of 6-8 weeks or more
Non-Surgical Treatment Options
Chemotherapy Regimens
Chemotherapy remains a cornerstone of MPM treatment, often using a combination of pemetrexed and cisplatin.
Pros of Chemotherapy in MPM Management
- Can shrink tumors by 20-40% in responsive patients
- Improves median survival by 2-3 months compared to supportive care alone
- Applicable to most patients, including those ineligible for surgery
Cons and Side Effects of Chemotherapy
- Response rates limited to 30-40% of patients
- Significant side effects including fatigue, nausea, and increased infection risk
- Limited long-term survival benefit, with median overall survival of 12-16 months
Radiation Therapy Approaches
Radiation can be used palliatively or as part of multimodal treatment strategies.
Advantages of Radiation Treatment
- Effective for pain control in up to 60% of patients
- Can be precisely targeted to reduce damage to healthy tissue
- Potential to improve local control when combined with surgery
Disadvantages and Potential Risks
- Limited effect on overall survival when used alone
- Risk of radiation pneumonitis in 5-15% of patients
- May cause fatigue and skin irritation in treated areas
Key Prognostic Factors in Malignant Pleural Mesothelioma
Tumor Characteristics
Cell Type Impact on Survival
Epithelioid type has the best prognosis, with median survival of 12-27 months compared to 4-18 months for sarcomatoid.
Stage at Diagnosis and Its Influence
Early-stage (I-II) patients have a median survival of 19-21 months, while advanced stages (III-IV) see 12-16 months.
Patient-Related Factors
Age and Overall Health Considerations
Patients under 65 with good performance status have 50% higher 2-year survival rates than older or less fit individuals.
Genetic and Molecular Markers
BAP1 mutations are associated with improved prognosis, with some studies showing up to 7 months longer median survival.
Side-by-Side Comparison: Surgical vs. Non-Surgical Approaches
Efficacy in Tumor Control
Surgery offers more complete tumor removal (70-95% for EPP, 60-80% for P/D) compared to chemotherapy’s 30-40% response rate.
Impact on Patient Survival
Multimodal treatment including surgery can extend median survival to 20-29 months, versus 12-16 months for chemotherapy alone.
Effect on Symptom Management
Both approaches can improve symptoms, with surgery potentially offering longer-lasting relief in 60-70% of cases, while chemotherapy and radiation provide palliative benefits in 40-60% of patients.
Recovery Time and Long-Term Quality of Life
Surgical approaches require longer initial recovery (4-8 weeks) but may offer improved long-term quality of life for responders. Non-surgical options have shorter recovery periods but may require ongoing treatment cycles.
Conclusion
Navigating the Complex Landscape of Mesothelioma Treatment
The journey through malignant pleural mesothelioma prognosis reveals a landscape of tough choices and careful considerations. Surgical options like P/D and EPP offer hope for extended survival but come with significant risks and recovery time. On the flip side, non-surgical approaches provide wider applicability and fewer immediate risks, yet often yield more modest survival gains. The key lies in personalized decision-making, weighing factors like tumor characteristics, overall health, and quality of life goals. Emerging therapies and ongoing research continue to reshape the playing field, offering new hope for improved outcomes. Ultimately, the “best” approach isn’t one-size-fits-all but rather a tailored strategy that aligns with individual circumstances and preferences. By staying informed and working closely with a specialized medical team, patients can navigate this challenging terrain with greater confidence, making choices that optimize their unique path forward in the face of this formidable disease.