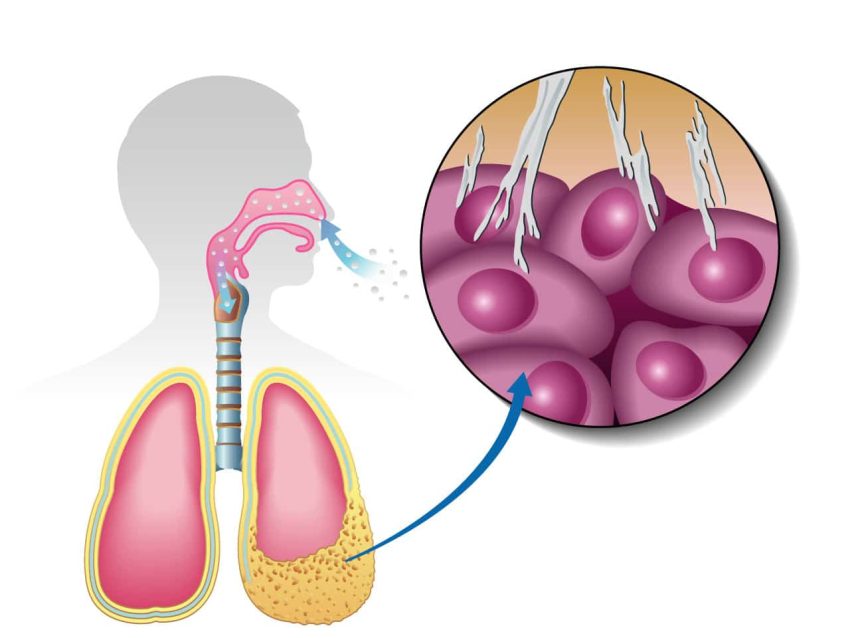
Pleural mesothelioma metastasis sites can significantly impact a patient’s prognosis and treatment options. As this aggressive cancer spreads, it often targets lymph nodes and the liver, each presenting unique challenges and considerations. Understanding the differences between these common metastatic locations is crucial for both patients and healthcare providers. This article delves into the characteristics, detection methods, and implications of lymph node and liver metastases in pleural mesothelioma. By comparing these two sites, we’ll explore how they influence disease progression, treatment approaches, and overall patient outcomes. Whether you’re navigating a recent diagnosis or seeking to expand your knowledge, this comprehensive comparison will shed light on the complex journey of mesothelioma metastasis.
Lymph Node Metastasis in Pleural Mesothelioma
Characteristics of Lymph Node Metastasis
Lymph node metastasis in pleural mesothelioma typically occurs through lymphatic spread. This process involves cancer cells breaking away from the primary tumor and traveling through lymph vessels to nearby lymph nodes. Studies show that approximately 40-50% of pleural mesothelioma patients present with lymph node involvement at diagnosis.
The most commonly affected lymph node regions include:
- Intrathoracic nodes (70-80% of cases)
- Mediastinal nodes (50-60% of cases)
- Hilar nodes (30-40% of cases)
Advantages of Lymph Node Metastasis Detection
Early detection of lymph node metastasis can significantly impact patient outcomes. Research indicates that patients with identified lymph node involvement have a median survival of 16.8 months compared to 24.6 months for those without lymph node metastasis.
Key benefits include:
- Improved staging accuracy (94% accuracy with PET-CT scans)
- More precise treatment planning
- Potential for targeted therapies
Challenges in Managing Lymph Node Metastasis
Despite the advantages of early detection, lymph node metastasis presents several challenges:
- Complete surgical removal is often difficult, with a success rate of only 60-70%
- Increased risk of local recurrence (40% within 2 years)
- Reduced effectiveness of radiation therapy due to widespread distribution
Liver Metastasis in Pleural Mesothelioma
Patterns of Liver Metastasis
Liver metastasis occurs through hematogenous spread, where cancer cells travel through the bloodstream. This form of metastasis is less common than lymph node involvement, affecting approximately 15-20% of pleural mesothelioma patients during their disease course.
Key characteristics include:
- Usually occurs in later stages of the disease
- Often accompanied by metastases to other distant organs (60% of cases)
- Tends to form multiple small lesions rather than a single large tumor
Benefits of Identifying Liver Metastasis
Recognizing liver metastasis is crucial for:
- Accurate disease staging (upstaging to Stage IV in 100% of cases)
- Guiding treatment decisions (palliative vs. curative intent)
- Predicting prognosis (median survival of 6-9 months with liver metastasis)
Complications Associated with Liver Metastasis
Liver metastasis in pleural mesothelioma often leads to:
- Reduced liver function (affecting up to 80% of patients)
- Increased treatment toxicity
- Limited options for systemic therapies (30-40% response rate to standard chemotherapy)
Key Comparison Factors
Diagnostic Imaging Techniques
PET-CT scans show high sensitivity for both lymph node (90-95%) and liver metastases (85-90%). However, MRI proves superior for liver lesions, detecting up to 97% of metastases smaller than 1 cm.
Impact on Disease Progression
Lymphatic spread tends to be slower, with a median time to progression of 9-12 months. Hematogenous spread to the liver is often more aggressive, with a median time to progression of 3-6 months.
Treatment Approaches
Surgical options for lymph node metastases include extended pleurectomy/decortication, with a 5-year survival rate of 15-20%. Liver metastases are generally not amenable to surgery, with systemic therapy being the primary approach (response rates of 30-40%).
Side-by-Side Comparison
| Factor | Lymph Node Metastasis | Liver Metastasis |
|---|---|---|
| Frequency | 40-50% at diagnosis | 15-20% during disease course |
| Detection Method | PET-CT (90-95% sensitivity) | MRI (97% sensitivity for small lesions) |
| Median Survival | 16.8 months | 6-9 months |
| Treatment Options | Surgery + Radiation | Primarily Systemic Therapy |
| Impact on Staging | Stage III | Stage IV |
This comprehensive comparison highlights the significant differences between lymph node and liver metastases in pleural mesothelioma. Understanding these distinctions is crucial for tailoring treatment strategies and managing patient expectations in the face of this challenging disease.
Conclusion
Understanding the nuances of pleural mesothelioma metastasis sites is crucial for patients and healthcare providers alike. While lymph node involvement offers a slightly more optimistic outlook with potential surgical interventions, liver metastasis often signals a more aggressive disease course. The choice between focusing on lymphatic or hematogenous spread isn’t binary; rather, it’s about tailoring treatment strategies to individual cases. Patients should work closely with their oncology team to interpret imaging results and weigh the pros and cons of various treatment approaches. As research advances, we may see more targeted therapies for specific metastatic patterns. For now, early detection remains key, regardless of the metastatic site. By staying informed about the characteristics of different metastasis locations, patients can better navigate their treatment journey and make informed decisions. Ultimately, the goal is to balance quality of life with the most effective treatment options available, considering the unique challenges posed by each metastatic site.