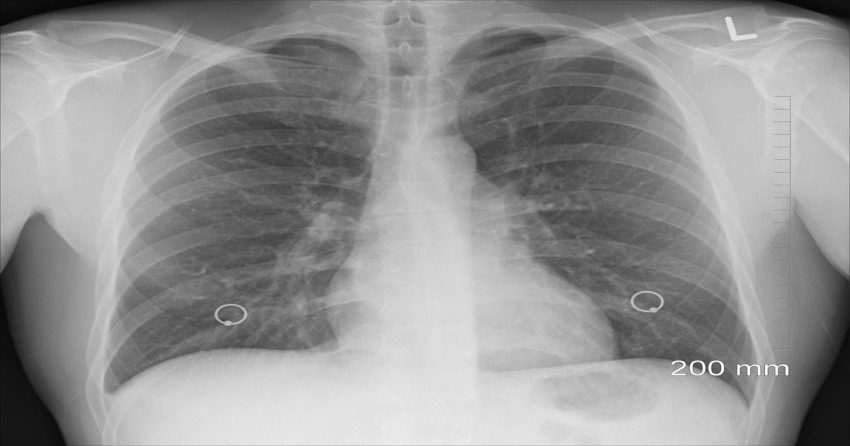
Pleural effusion, a common complication of mesothelioma, can be a daunting challenge for patients and caregivers alike. This buildup of fluid around the lungs often leads to breathlessness and discomfort, significantly impacting quality of life. But don’t lose heart – knowledge is power, and understanding this condition is the first step towards effective management. In this guide, we’ll walk you through the ins and outs of pleural effusion in mesothelioma, from recognizing symptoms to exploring treatment options. Whether you’re newly diagnosed or supporting a loved one, you’ll find practical tips, expert insights, and compassionate advice to help navigate this complex journey. Let’s dive in and empower ourselves with the information needed to face pleural effusion head-on.
Key Information for Patients and Caregivers
When dealing with pleural effusion in mesothelioma, having the right resources at your fingertips can make a world of difference. This section is your go-to toolkit, packed with essential info to help you navigate this challenging journey. From decoding medical jargon to finding top-notch support, we’ve got you covered. Let’s explore the must-have knowledge and resources that’ll empower you to take charge of your health or support your loved one effectively.
Essential Medical Terminology
Getting a grip on medical lingo can feel like learning a new language, but don’t sweat it! We’ll break down the key terms you’ll encounter:
- Pleura: The thin membrane lining your lungs and chest cavity
- Thoracentesis: A procedure to drain excess fluid from the pleural space
- Pleurodesis: A treatment to prevent fluid buildup by sealing the pleural space
- Dyspnea: The medical term for shortness of breath
Understanding these terms will help you communicate more effectively with your healthcare team and feel more in control of your situation.
Recommended Resources for Further Reading
Knowledge is power, especially when it comes to managing pleural effusion and mesothelioma. Here are some trustworthy sources to expand your understanding:
- American Cancer Society’s Mesothelioma Guide
- Mesothelioma Applied Research Foundation
- National Cancer Institute’s Mesothelioma Information
These resources offer in-depth information on symptoms, treatments, and the latest research, helping you make informed decisions about your care.
Important Contact Information
Having the right contacts can be a lifeline during your mesothelioma journey. Here’s a list of essential connections:
- Mesothelioma specialists in your area
- Local support groups for mesothelioma patients and caregivers
- Asbestos exposure legal advisors
- Palliative care services
Remember, you’re not alone in this fight. Reaching out to these resources can provide invaluable support, guidance, and care when you need it most.
Navigating Your Mesothelioma Journey: From Diagnosis to Management
Dealing with pleural effusion and mesothelioma can feel overwhelming, but taking it step-by-step can make the process more manageable. Let’s break down this journey into clear, actionable stages to help you or your loved one navigate the path ahead with confidence and clarity.
Recognizing the Signs
The first step in tackling pleural effusion is knowing what to look out for:
- Pay attention to persistent shortness of breath
- Note any chest pain, especially when breathing deeply
- Be aware of a dry, nagging cough that won’t go away
- Monitor for unexplained fatigue or weight loss
Tip: Keep a symptom diary to track changes over time. This can be invaluable when discussing your condition with healthcare providers.
Warning: Don’t ignore these symptoms, especially if you have a history of asbestos exposure. Early detection can make a significant difference in treatment outcomes.
Seeking Medical Attention
Once you’ve noticed concerning symptoms, it’s crucial to take action:
- Schedule an appointment with your primary care physician
- Prepare a list of your symptoms and medical history
- Be ready to discuss any potential asbestos exposure
- Ask for a referral to a mesothelioma specialist if necessary
Tip: Bring a friend or family member to your appointments. They can provide support and help remember important information.
Warning: Avoid self-diagnosing or delaying medical care. Pleural effusion can have various causes, and professional evaluation is essential.
Undergoing Diagnostic Tests
Your healthcare team will likely recommend several tests to confirm the diagnosis:
- Chest X-ray to visualize fluid buildup
- CT scan for a more detailed view of the lungs and pleura
- Thoracentesis to analyze the pleural fluid
- Biopsy to confirm mesothelioma if suspected
Tip: Don’t hesitate to ask questions about each procedure and what to expect.
Warning: Some tests may cause temporary discomfort. Communicate any concerns with your medical team to ensure your comfort throughout the process.
Conclusion
Navigating the complex landscape of pleural effusion in mesothelioma requires courage, knowledge, and a proactive approach. By understanding the symptoms, seeking timely medical attention, and actively participating in your treatment journey, you’ve taken crucial steps towards managing this challenging condition. Remember, while the road ahead may seem daunting, you’re not walking it alone. The advancements in medical science, coupled with support from healthcare professionals and loved ones, offer hope and improved quality of life. As you move forward, stay informed, advocate for yourself, and don’t hesitate to lean on your support network. Your resilience in facing this challenge is commendable, and each day brings new possibilities in mesothelioma research and treatment. Embrace a positive outlook, focus on self-care, and continue to fight with determination. Your journey is unique, and your strength in navigating it is inspiring.
Additional Tips/FAQs
Q: Can lifestyle changes help manage pleural effusion symptoms?
A: Absolutely. Gentle exercise, proper nutrition, and stress reduction techniques can complement medical treatments and improve overall well-being.
Q: Is it normal to feel overwhelmed by the diagnosis?
A: Yes, it’s entirely normal. Seek emotional support through counseling or support groups to help cope with the psychological impact.
Q: How often should I follow up with my doctor?
A: Follow-up frequency varies, but regular check-ins are crucial. Discuss a personalized follow-up schedule with your healthcare team.
Tip: Keep a updated list of all medications and treatments to share with your medical team during appointments.
Tip: Consider joining a mesothelioma research study. It could provide access to cutting-edge treatments while contributing to scientific advancement.